table of contents

Type 1 diabetes (T1D) is a chronic autoimmune disease that affects millions of people worldwide. Unlike type 2 diabetes, which is often linked to lifestyle factors, type 1 diabetes occurs when the body’s immune system mistakenly attacks insulin-producing beta cells in the pancreas. This leads to a complete lack of insulin, a hormone essential for regulating blood sugar levels. Without insulin, glucose cannot enter cells to provide energy, leading to high blood sugar (hyperglycemia) and serious health complications.
In this article, we will explore the causes, symptoms, progression, and available treatment options for type 1 diabetes.
Causes of Type 1 Diabetes
The exact cause of type 1 diabetes remains unclear, but researchers believe it results from a combination of genetic and environmental factors.
- Autoimmune Reaction
Type 1 diabetes is classified as an autoimmune disorder, meaning the body’s immune system mistakenly attacks its own cells. In this case, the immune system destroys the insulin-producing beta cells in the pancreas.
According to Dr. Richard Insel, former Chief Scientific Officer at the Juvenile Diabetes Research Foundation (JDRF):
“Type 1 diabetes is triggered by an autoimmune reaction that leads to the destruction of insulin-producing cells. This process often starts months or even years before symptoms appear.”
- Genetic Factors
Individuals with a family history of type 1 diabetes have a higher risk of developing the condition. Scientists have identified certain genes, such as those in the HLA (human leukocyte antigen) complex, that increase susceptibility.
A study published in Diabetes found that first-degree relatives of people with type 1 diabetes have a 15 times higher risk of developing the disease compared to the general population.
- Environmental Triggers
Environmental factors, such as viral infections, may play a role in triggering the immune response that leads to type 1 diabetes. Researchers have studied viruses like enteroviruses, coxsackieviruses, and Epstein-Barr virus as potential triggers.
Dr. Jessica Dunne, Director of Research at JDRF, states:
“While genetic predisposition plays a role, we know that environmental factors such as viral infections and gut microbiome imbalances contribute to the development of type 1 diabetes.”

Symptoms of Type 1 Diabetes
The symptoms of type 1 diabetes often develop rapidly, especially in children and young adults. Recognizing these early warning signs is crucial for timely diagnosis and treatment.
Common Symptoms Include:
- Excessive thirst (polydipsia) – Constantly feeling thirsty despite drinking fluids
- Frequent urination (polyuria) – The need to urinate more often, even at night
- Unexplained weight loss – Despite normal or increased appetite
- Extreme fatigue – Persistent tiredness and lack of energy
- Blurred vision – Due to fluid imbalances affecting the eyes
- Slow-healing wounds and infections – Cuts and infections take longer to heal
- Fruity-smelling breath – A sign of diabetic ketoacidosis (DKA), a life-threatening condition
If left untreated, type 1 diabetes can lead to diabetic ketoacidosis (DKA), a serious condition characterized by dangerously high blood sugar, dehydration, and acid buildup in the blood.
Progression of Type 1 Diabetes
The progression of type 1 diabetes occurs in stages:
- Stage 1: Autoimmune markers are present, but blood sugar levels are still normal, and there are no symptoms.
- Stage 2: Blood sugar levels start to rise, but symptoms remain mild or unnoticed.
- Stage 3: Symptoms become apparent, leading to diagnosis. At this stage, insulin production is significantly reduced or absent.
A study published in The Lancet Diabetes & Endocrinology highlights that type 1 diabetes may begin years before symptoms appear, with detectable autoantibodies present in high-risk individuals.
Treatment and Management of Type 1 Diabetes
While there is currently no cure for type 1 diabetes, advancements in medical treatment have significantly improved disease management and quality of life.
- Insulin Therapy
Since type 1 diabetes results in little to no insulin production, insulin therapy is essential. There are several types of insulin, including:
- Rapid-acting insulin (e.g., Lispro, Aspart) – Works quickly to manage blood sugar spikes
- Short-acting insulin (e.g., Regular insulin) – Used before meals
- Intermediate-acting insulin (e.g., NPH) – Provides longer-lasting blood sugar control
- Long-acting insulin (e.g., Glargine, Detemir) – Maintains baseline insulin levels throughout the day
Dr. Irl Hirsch, an endocrinologist at the University of Washington, emphasizes:
“Insulin therapy has advanced significantly, and with the use of continuous glucose monitors (CGMs) and insulin pumps, patients can achieve much better blood sugar control.”
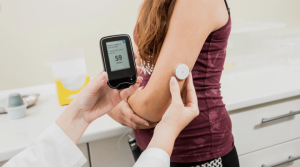
- Continuous Glucose Monitoring (CGM)
CGMs, such as Glucofit, provide real-time glucose readings, helping patients track blood sugar fluctuations and adjust insulin doses accordingly.
A study published in The New England Journal of Medicine found that CGM users experience fewer hypoglycemic episodes and improved overall blood sugar control.
- Artificial Pancreas Technology
The development of automated insulin delivery systems, also known as artificial pancreas systems, has revolutionized type 1 diabetes management. These devices use CGMs and insulin pumps to automatically adjust insulin delivery based on real-time glucose levels.
- Lifestyle Modifications
While type 1 diabetes is not caused by diet or lifestyle, healthy habits play a crucial role in blood sugar control:
✅ Balanced Diet: A diet rich in fiber, healthy fats, and lean proteins helps prevent blood sugar spikes.
✅ Regular Exercise: Physical activity improves insulin sensitivity and overall metabolic health.
✅ Stress Management: Stress can elevate blood sugar levels, making relaxation techniques like meditation beneficial.
- Future Treatments and Research
Researchers are exploring innovative treatments such as:
- Beta cell regeneration: Scientists are working on therapies to regenerate insulin-producing cells.
- Immunotherapy: Clinical trials are testing immune-modulating drugs to prevent or slow disease progression.
- Stem cell therapy: Efforts are underway to develop stem cell-based insulin-producing cells for transplantation.
According to Dr. Aaron Kowalski, CEO of JDRF:
“We are at a turning point in type 1 diabetes research, with promising developments in beta cell replacement therapy and immune interventions that could change the future of this disease.”

Conclusion
Type 1 diabetes is a lifelong condition that requires careful management, but with advances in insulin therapy, glucose monitoring, and emerging treatments, individuals with T1D can lead full and healthy lives.
Early diagnosis, personalized treatment, and the latest technologies—such as CGMs and artificial pancreas systems—are improving patient outcomes and quality of life.
For those managing type 1 diabetes, tracking blood sugar levels with innovative tools like Glucofit provides valuable insights, helping individuals maintain better control and reduce the risk of complications.
Would you like to learn more about how Glucofit can help manage blood sugar levels? Take control of your diabetes today!


